Updated on May 6, 2026

Key Takeaways
- • AI in the insurance market is valued at $13.45 billion in 2026 and continues to accelerate across claims, underwriting, and customer experience (Fortune Business Insights, 2026).
- • Conversational AI in insurance is growing at 32.3% CAGR, projected to reach $246.3 billion by 2035 (Market Research Future, 2026).
- • Enterprise deployments require compliance specifics: SOC 2 Type II, HIPAA, GDPR, and ISO 27001 — not just chatbot functionality.
- • A Minimum Viable Agent (MVA) pilot can go live in 30 days by targeting five high-volume intents first, then expanding from real data.
- • ROI is best measured across five KPIs: containment rate, cost per contact, first response time, CSAT, and renewal conversion rate.
Insurance carriers have invested heavily in digital transformation. Yet for many policyholders, support still feels slow and fragmented: IVR menus, portal logins, and email threads that stall exactly when help is most urgent.
If a customer has a question about a premium change or needs to file a First Notice of Loss (FNOL) on a weekend, they rarely want to download a new app or wait days for a response. They want immediate, accurate guidance and a clear next step.
In other words: policyholders want fast answers in the channels they already use.
This expectation gap is structural. Mobile is now the primary way billions access online services, and messaging has become a default interface for support. But many insurance experiences still force customers into disconnected systems. Conversational AI can provide a persistent conversation layer across the full policy lifecycle.
To modernize insurance support without losing compliance control, insurers need full-funnel journeys and governance-by-design. This article outlines a practical approach, including a 30-day pilot plan and an ROI measurement framework. We cover:
1. What is Conversational AI in Insurance?
2. Why does the Insurance Industry need Conversational AI now?
3. How Have Policyholder Expectations Changed?
4. What Tasks Should Conversational AI in Insurance Perform?
5. What Are the High-Impact Use Cases of Conversational AI in Insurance?
6. Benefits of Conversational AI for Insurance Companies
7. How Do You Ensure Control, Governance, and Compliance?
8. Why Do You Need System Integrations During This Process?
9. How Can You Roll Out a Conversational AI Pilot in Insurance in 30 Days?
10. How Should Leaders Measure ROI?
10. Where Does Kommunicate Fit in the Solution Stack?
11. What Common Failure Modes Should You Avoid?
12. Conclusion
13. Frequently Asked Questions (FAQs)
What is Conversational AI in Insurance?
Conversational AI in insurance refers to AI-powered systems: chatbots, voice agents, and virtual assistants that interact with policyholders and agents using natural language, whether through text, voice, or messaging apps. These systems handle everything from answering policy questions to processing claims, without requiring a customer to navigate phone trees or wait for business hours.
The technology combines natural language processing (NLP), machine learning, and dialogue management to understand customer intent, maintain context across a multi-turn conversation, connect to backend systems, and take action.
These modern AI systems for insurance differ significantly from traditional chatbots.
How are Conversational AI Systems in Insurance Different from Basic Chatbots?
Operationally speaking, a chatbot follows a pre-written script and breaks the moment a customer phrases something unexpectedly. But a conversational AI agent understands intent, maintains context across a full conversation, and connects to live systems to take action.
| Basic Chatbot | Conversational AI Agent | |
|---|---|---|
| Understanding | Fixed scripts, keyword matching | NLP-based intent recognition, handles natural phrasing |
| Context | Resets each message | Maintains full conversation context and history |
| Capabilities | Answers FAQs, links to help articles | Processes claims, updates policies, generates quotes |
| Integration | Standalone | Connected to CRM, policy admin, claims, billing systems |
| Escalation | Transfers call, loses context | Transfers with full transcript and pre-filled context |
| Learning | Static | Improves over time from interaction data |
Kommunicate was built using the latest NLP tools to make conversational AI agents generally accessible. And while our primary interface still is the web chatbot, its capabilities are vastly different (and improved) from the chatbots of old.
Recently, we have worked with large enterprise clients in insurance, and that has convinced us that conversational AI will play a large part in changing the policyholder journey.
Why does the Insurance Industry need Conversational AI now?
The business case for conversational AI in insurance is no longer speculative. Market adoption, customer data, and operational pressures have converged to make it a strategic necessity.
Market Size and Opportunity
| AI in the insurance market is valued at $13.45 Billion in 2026 (Fortune Business Insights, 2026). |
| Conversational AI in insurance is growing at 32.3% CAGR, projected to reach $246.3 B by 2035 (Market Research Future, 2026). |
| 18% of Insurance executives say that AI has already reached the scaling phase in knowledge management and service operations. (McKinsey, 2025) |
| Insurance companies that currently lead in digital and AI adoption outperform their competitors by 6.1x. (Mckinsey, 2024). |
These market conditions have created a unique combination of pressure on C-level insurance executives.
The Current Imperative for the Insurance Industry
Four specific pressures are pushing insurers to move now rather than later:
- Customer expectations have permanently shifted. Policyholders benchmark their insurer against every digital experience they have.
When they can track a delivery in real time but cannot get a claim status update without calling during business hours, trust erodes. - Volume is outpacing human capacity. A mid-sized insurer handling 50,000 monthly inquiries cannot scale by hiring indefinitely. Claims alone generate enormous call volume: FNOL, status checks, document requests, and payment questions, each requiring agent time for what is often a two-minute lookup. Most insurance firms see a 30–50% reduction in routine support volume after implementing conversational AI (Rasa).
- Cost pressure is relentless. Gartner reports an average of $8.01 per live-agent contact (2019). Automated resolution costs a fraction of that. Every routine query handled by AI is direct margin recapture.
- Retention depends on service quality. Research shows 83% of consumers would consider switching insurers after a poor claims experience (InvoiceCloud & Konecta, 2026).
- Conversational AI enables instant acknowledgement, real-time status updates, and proactive communication: the exact factors that prevent churn at renewal.
These factors indicate that the high level of competition and increasing margin pressures have been at the heart of the conversational AI in insurance expansion. But, these factors are being escalated by a change in policyholder behavior and expectations.
How Have Policyholder Expectations Changed?
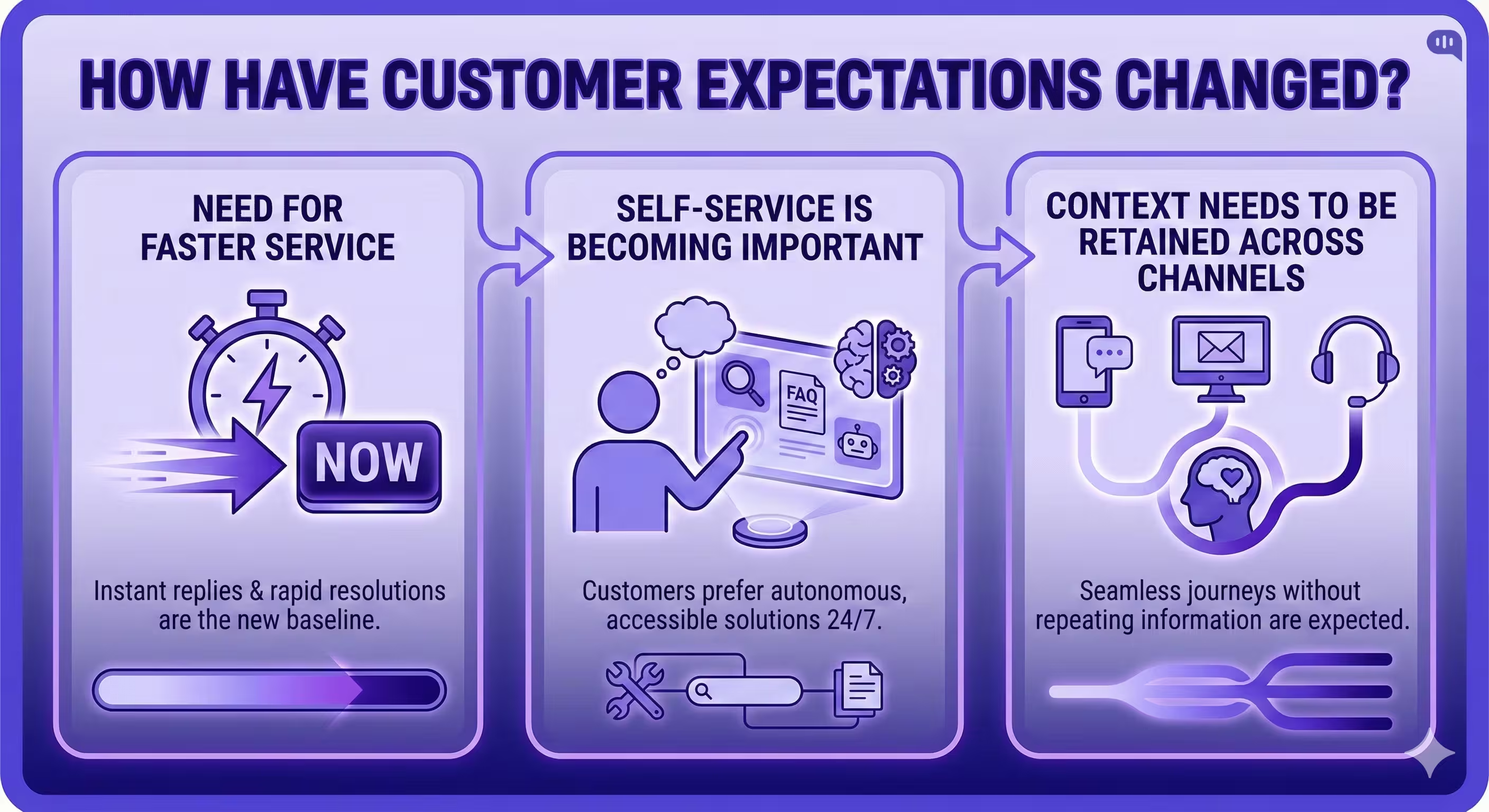
The modern policyholder doesn’t view calling support as a “channel”—they view it as a failure of the digital experience. Here are the three non-negotiables defining the new baseline for insurance service:
1. Customers Expect Faster Service
Speed is no longer a “good-to-have”; it is the primary driver of retention. In the on-demand economy, the tolerance for “we’ll get back to you in 24–48 hours” has evaporated.
- The Cost of Delay: Policyholders increasingly expect 24/7 availability and rapid issue resolution—especially during high-stress events like a claim. When updates take days, customers assume the insurer is not in control.
- The AI Benchmark: Some insurers have reset expectations with automation. Lemonade reports that as of December 31, 2024, its claims bot (AI Jim) handled the first notice of loss without human intervention 96% of the time. At scale, conversational automation can also reduce call center load—Vodafone reported a 12% year-on-year reduction in the frequency of customer contacts to its call centres in Q4 after deploying AI chatbots across markets.
- The Takeaway: If your FNOL process takes days to acknowledge, you are already losing the renewal battle.
2. Self-Service Channels are Becoming Important
For years, insurers treated self-service as a cost-cutting measure to “deflect” calls. Today, it is a genuine customer preference.
- Autonomy Is Preferred: Policyholders increasingly want to resolve routine issues on their own—without waiting on hold or navigating multiple handoffs. When self-service is missing or incomplete, they either abandon the journey or shift to assisted channels.
- High Resolution Potential: This is not limited to static FAQs. When connected to the right systems, conversational AI can handle end-to-end tasks like answering policy questions, collecting claim details, checking status, and triggering approved workflows—while escalating edge cases to humans.
- Proactivity Wins: Customers also expect timely, proactive updates—especially during claims and renewals. Automated notifications (status changes, missing documents, payment reminders) reduce inbound “check-in” contacts and improve perceived transparency.
3. Customers Expect You to Retain Context Across Channels
“Omnichannel” is often a buzzword for “being everywhere,” but to a customer, it means “remembering everything.”
- “Repeat” Fatigue: One of the fastest ways to lose trust is forcing a customer to repeat themselves across channels or agents. The more emotional the moment (for example, a claim), the more damaging this feels.
- The Context Gap: If a customer starts a claim on WhatsApp and then calls your support line, they expect the agent to see the photos they just uploaded. When that context is lost, trust erodes.
- True Omnichannel: It is not enough to simply have a web chat and a phone line. The “new baseline” is a shared conversation history where the context travels with the user, ensuring that whether they are on an app, a website, or a call, the conversation picks up exactly where it left off.
To meet these rising expectations, insurance carriers must move beyond simple FAQs and deploy AI agents that can actually “do” work, not just talk about it. Next, we will break down exactly which capabilities separate a helpful digital assistant from a glorified search bar.
What Tasks Should Conversational AI in Insurance Perform?
A modern AI agent must serve as a transactional layer capable of executing complex workflows, not just a passive information retrieval tool. It should seamlessly handle the “heavy lifting” of insurance administration, freeing human agents for high-value empathy work.
| Feature | Benefit | Impact on Customer |
| Smart Authentication | Verifies identity via OTP or biometrics within the chat flow before sharing sensitive data. | Security without friction: No need to remember policy numbers or log into a separate portal just to check a status. |
| Instant Policy Retrieval | Fetches real-time status, premium due dates, and coverage limits directly from the core admin system. | Immediate clarity: Answers “Is this covered?” or “When is my payment due?” in seconds, 24/7. |
| Automated FNOL (First Notice of Loss) | Guides users through claim reporting, photo uploads, and location sharing in a conversational interface. | Stress reduction: Transforms a panicked, complex form-filling process into a simple, guided chat during a stressful moment. |
| Proactive Reminders & Nudges | Sends automated WhatsApp or SMS alerts for upcoming renewals, missed payments, or document expirations. | Peace of mind: Prevents accidental policy lapses and ensures continuous coverage without the customer having to track dates. |
| Seamless Human Handoff | Transfers the chat to a live agent with full transcript history and pre-filled context when complex issues arise. | Zero repetition: The customer never has to “start over,” feeling understood and valued even when the bot hits its limit. |
Modern insurance customers demand speed, self-service, and context retention, and they expect these across every channel they use. In the next section, let’s look at the five specific workflows where AI delivers the highest return on investment.
What Are the High-Impact Use Cases of Conversational AI in Insurance?
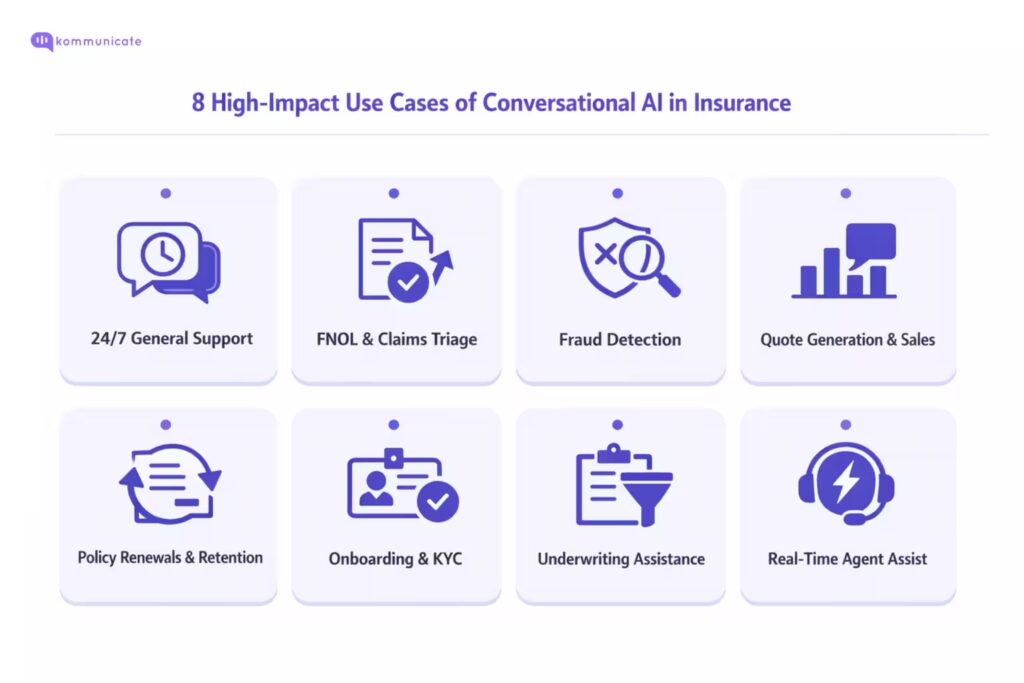
Many carriers make the mistake of trying to “boil the ocean” by automating everything at once. The better approach is to focus on these five high-friction journeys where AI can deliver immediate value.
1. General Support & FAQ Automation
This is the low-hanging fruit. A large share of inbound insurance queries are repetitive (coverage basics, documents, payment dates, claim status). Automating these frees human agents to focus on complex exceptions and high-empathy conversations.
Case Study: Conte.it
As one of Italy’s leading auto insurers, Conte.it faced a massive volume of repetitive calls from a diverse customer base—some tech-savvy, others preferring phones. They needed a way to offer autonomy without losing the personal touch.
Solution: They deployed a Kommunicate-powered chatbot to handle a majority of routine conversations. In the published deployment story, Conte.it reported ~90% automation and 4,300+ hours of manual work saved, while maintaining high availability for customers.
2. First Notice of Loss (FNOL) & Claims Triage
The “moment of truth” in insurance is the claim. Traditional FNOL involves waiting on hold while stressed. AI agents can turn this into a guided, empathetic chat workflow available 24/7.
Case Study: Lemonade
Instead of a phone tree, the user types “I had an accident.” The AI instantly empathizes, verifies safety, and then guides the user to upload photos, share GPS location, and voice-record a statement.
The Impact: Leading insurtechs like Lemonade using this model have reduced claim filing times from 20 minutes to 3 minutes, with simple claims (like glass damage) being approved instantly via algorithmic validation.
3. Lead Qualification & Quote Generation
Sales teams waste hours chasing cold leads. An AI agent acts as an always-on SDR (Sales Development Representative), engaging website visitors, answering pre-sales questions (“Does this cover flood damage?”), and generating instant quotes.
Case Study: AA Ireland
A visitor lands on a pricing page at 11 PM. The bot engages them, asks 4-5 qualifying questions (age, location, asset value), and provides an estimated premium. If the lead is high-value, the bot schedules a callback for the human sales team the next morning.
The impact: Automated qualification improves sales efficiency by capturing intent, answering common coverage questions, and routing only well-qualified prospects to agents. Measure lift through funnel completion rate, callback-to-close rate, and agent time saved.
4. Policy Renewals & Retention
Churn often happens simply because a customer missed an email. AI agents turn passive renewal notices into active, two-way conversations on channels like WhatsApp or SMS.
Case Study: Accenture
30 days before expiration, the AI sends a WhatsApp message: “Hi Alex, your auto policy expires soon. Your renewal quote is $800. Reply, ‘RENEW’ to process instantly.” If the user hesitates, the bot can ask, “Is price a concern?” and offer to adjust deductibles.
The impact: Renewal automation reduces involuntary churn by making it easier to pay, update details, and resolve last-mile questions before expiry. Personalization (based on policy type, region, and customer behavior) can also improve renewal completion rates—validate this in your pilot.
5. Onboarding & KYC
The drop-off rate during onboarding is high because collecting documents (IDs, proof of address) is tedious. AI agents can chase these documents asynchronously, verify them in real-time, and nudge users who stall.
Case Study: Penguin Securities
After a policy purchase, the AI messages the user: “We just need a photo of your driving licence to activate your policy. You can upload it right here.” The AI validates the image quality instantly, rejecting blurry photos before a human ever has to check.
The impact: Automated document collection and verification can compress onboarding timelines by removing back-and-forth and catching issues (missing fields, unreadable images) immediately. The exact improvement depends on your workflow and risk checks, so benchmark your current cycle time first.
6. Fraud Detection and Claims Integrity
Conversational AI contributes to fraud prevention at the intake stag. The system cross-references claim details against policy data and historical patterns in real time, flags inconsistencies (contradictory location data, mismatched timing, prior claims concentration), and captures a structured, verbatim statement from the claimant that can be reviewed later.
- Real-time pattern matching against policy terms and prior claim history
- Structured statement capture for evidentiary purposes
- Automatic flagging for human review when anomaly thresholds are exceeded
- Audit trail on every intake interaction for compliance and legal defence
Advanced implementations report fraud detection accuracy exceeding 99% at the intake stage (ResearchGate, 2026). The key advantage is that fraud signals are captured before human adjusters invest time — reducing both losses and investigative costs.
7. Underwriting Assistance
Conversational AI accelerates the underwriting process by handling data collection, document processing, and preliminary risk screening.
- Automated applicant data collection via guided conversational intake
- Document ingestion and OCR extraction from uploaded files (medical records, financial statements, vehicle inspections)
- Preliminary risk classification based on configured underwriting rules
- Missing information identification and automated follow-up
- Regulatory compliance monitoring — flagging decisions that may fall outside approved underwriting guidelines
The result is a reduction in underwriting cycle time from days to hours for standard risk profiles, with consistent data quality because the AI captures information in structured form from the outset. Human underwriters receive a pre-populated risk brief rather than a pile of unstructured documents.
8. Real-Time Agent Assist and Compliance Guidance
Conversational AI is not only a customer-facing layer. Deployed as an agent assist tool, it runs alongside live calls and chat conversations, surfacing the right information and guidance to human agents in real time — making every agent perform like your best agent.
- Next-best-action prompts based on customer query and policy data
- Real-time compliance reminders — surfacing required disclosures before an agent needs to remember them
- Auto-generated call summaries and CRM notes after each interaction
- Quality monitoring and coaching flags for training purposes
This use case is particularly valuable during the onboarding of new agents and during catastrophe events when experienced staff are stretched. The AI provides guardrails without slowing the conversation.
When you use conversational AI in insurance to automate the above processes, some benefits are directly passed onto your business.
Benefits of Conversational AI for Insurance Companies
The use cases above translate into five measurable business outcomes:
| Benefit | What It Means in Practice | Benchmark |
|---|---|---|
| 24/7 availability without proportional cost growth | AI handles the same query volume at 2 AM as at 2 PM — without overtime, staffing spikes, or degraded quality. | Scale to unlimited concurrent conversations |
| Faster claims resolution | FNOL intake reduced from 20 minutes to under 3 minutes. Initial processing time reduced by up to 80% (ResearchGate, 2024). | 80% reduction in initial processing time |
| Higher renewal rates | Proactive, personalised outreach on preferred channels converts passive renewal notices into active confirmations. | 30–50% reduction in involuntary churn |
| Full compliance audit trail | Every conversation is logged, structured, and searchable. Regulatory audits become a reporting exercise, not an investigation. | 100% of interactions documented |
| Improved agent productivity | Routine query deflection frees agents for complex, high-value conversations. Agent assist tools raise performance floor across the team. | 30–50% reduction in routine support volume |
How Do You Ensure Control, Governance, and Compliance?

In insurance, a “hallucination” isn’t just a funny AI glitch—it’s a lawsuit. Unlike retail or media, the insurance sector operates under strict regulatory frameworks where every word counts. A bot cannot simply “guess” coverage limits or give financial advice.
To move from a pilot to production, you need an architecture designed for zero-trust security and determinism. This means the AI must know what it cannot say just as well as what it can.
The “Refusal” Layer: What the Agent Must Not Answer
Your AI agent needs strict guardrails (hard refusal rules). It should be designed to decline unsafe, non-compliant, or out-of-scope requests, and to escalate to a human when the customer’s situation requires judgment or policy interpretation beyond approved language.
- Example: If a user asks for help falsifying a claim or bypassing eligibility checks, the agent must refuse and direct the customer to compliant channels (or escalate to a human reviewer as per your policy).
- Implementation: Use a whitelist approach where the bot is only allowed to pull answers from approved knowledge sources (policy documents, SOPs, and legal wordings), ignoring general internet knowledge.
Enterprise-Grade Security Certifications
You cannot integrate with core insurance systems (PAS, Claims DB) without meeting global security standards. Ensure your conversational AI platform checks these boxes:
- SOC 2 Type II: A widely adopted assurance standard for SaaS providers. It demonstrates that a vendor’s controls around security, availability, and confidentiality have been independently assessed over a period of time.
- GDPR & HIPAA Compliance: If you handle health insurance or operate in the EU, the platform must support data masking (redacting PII like SSNs or medical diagnoses) and the “Right to be Forgotten.”
- ISO 27001: This international standard ensures the vendor has a rigorous Information Security Management System (ISMS) in place.
Data Privacy & PII Handling
Insurance conversations are laden with Personally Identifiable Information (PII). A secure AI agent must handle this data without storing it permanently in the chat logs.
- Data Masking: Automatically redact sensitive fields (credit card numbers, DOBs, SSNs) in the agent dashboard so human supervisors see [REDACTED] instead of raw data.
- Data Residency: Ensure your provider offers data hosting in your specific region (e.g., EU-only servers) to comply with data sovereignty laws.
- Encryption: Look for AES-256 encryption for data at rest and TLS 1.2+ for data in transit.
Governance establishes the trust required to interact with customers, but deep system integration gives your AI the power to actually serve them. Next, we explore why your AI is only as smart as the systems it connects to.
Why Do You Need System Integrations During This Process?
If your AI agent isn’t connected to your backend systems, it is nothing more than a glorified FAQ page. It can tell a customer how to file a claim, but it can’t help them actually do it.
“AI is the interface; your systems are the engine.” To move from passive information delivery to active resolution, your conversational layer must plug directly into your existing tech stack (CRM, Policy Admin Systems, Claims Databases).
Here is how deep integration transforms the effectiveness of your AI:
- It Eliminates “Triage Fatigue”: By integrating with your CRM (like Pipedrive or Salesforce), the AI instantly recognizes the returning customer. Instead of asking generic questions (“What is your name?”), it opens with personalized context: “Welcome back, Sarah. Are you asking about the claim you filed last Tuesday?”
- It Enables Real-Time Transactions: Connection to your Policy Admin System (PAS) allows the AI to fetch live data rather than static text. It can pull up specific premium amounts, renewal dates, and deductible limits in milliseconds, ensuring the customer gets their answer, not a generic one.
- It Closes the Revenue Loop: Integrating with Payment Gateways (like Stripe or Razorpay) turns the chat window into a point of sale. The AI can generate a quote, serve a payment link, and confirm receipt of funds all within the same conversation thread, reducing drop-off during renewals.
- It Automates the Paperwork: Links to Document Management Systems (DMS) and OCR tools allow the AI to accept file uploads (like accident photos or IDs), automatically attach them to the correct customer record, and verify them for clarity without human intervention.
- It Empowers Human Agents: When integration extends to your Helpdesk Software (like Zendesk or Freshdesk), a bot escalation doesn’t just dump the user in a queue. It creates a ticket, populates it with the full chat transcript and recognized intent, and presents it to the human agent so they can solve the issue immediately.
Integration transforms your AI from a passive knowledge base into an active member of your workforce, capable of resolving issues rather than just describing them.
To summarize, this is how integrations work across the insurance tech stack:
| System | What Integration Enables |
|---|---|
| CRM (Salesforce, Pipedrive) | Instant customer recognition on inbound contact. Instead of “What is your policy number?”, the AI opens with “Welcome back, Sarah, are you calling about the claim you filed on Tuesday?” |
| Policy Admin System (PAS) | Real-time data retrieval: specific premium amounts, renewal dates, coverage limits, deductible status. The customer gets their answer, not a generic approximation. |
| Claims Database | Live claim status, adjuster assignment, missing document flags, payment timeline |
| Payment Gateway (Stripe, Razorpay) | The AI generates a renewal quote, serves a payment link, confirms payment receipt, and updates the policy record |
| Document Management / OCR | Accepts photo uploads, attaches them to the correct customer record, validates image quality, and flags missing or unreadable documents immediately. |
| Helpdesk (Zendesk, Freshdesk) | When the AI escalates, it creates a pre-populated ticket with the full transcript, recognised intent, and relevant policy data |
You don’t need to rebuild your entire tech stack to get started. In fact, the most successful carriers start small and scale fast.
How Can You Roll Out a Conversational AI Pilot in Insurance in 30 Days?
The biggest mistake insurers make is spending six months trying to build a “Death Star”—an AI that answers everything. By the time it launches, customer needs have changed, and the project is over budget.
A better approach is the “Minimum Viable Agent” (MVA). The goal is to prove value in one specific area (like “Claims Status” or “Renewal FAQs”) within four weeks. This creates momentum and generates the real-world data needed to expand safely.
Here is a pragmatic 30-day roadmap to get your first AI agent live:
| Timeline | Jobs to be Done | Relevant KPIs | Owners |
| Week 1: Strategy & Scope | • Select top 5 high-volume intents (e.g., “Status Check,” “Premium Due Date”) to automate. • Define “No-Go” zones (topics the bot must refuse). • Map the escalation path (who takes over when the bot fails?). | • Estimated Deflection Rate • Scope Freeze | • Product Manager • CS Lead |
| Week 2: Build & Connect | • Ingest existing FAQs and policy docs into the knowledge base. • Build the conversation flow for the top 5 intents. • Integration Lite: Connect one read-only system (e.g., check status via API). | • Intent Recognition Accuracy (Target >85%) • System Latency | • Implementation Engineer • Content Writer |
| Week 3: Internal Pilot (UAT) | • Staff Testing: Have your support team try to “break” the bot. • Refine answers based on “hallucinations” or confusion. • Verify PII masking and security logs. | • False Positive Rate • User Acceptance Score | • QA Team • Compliance Officer |
| Week 4: Soft Launch | • Deploy on a single low-risk channel (e.g., specific web page or post-login). • Direct only 10–20% of traffic to the bot. • Monitor “Fallbacks” (bot didn’t understand) daily and retrain. | • Containment Rate • CSAT (Customer Satisfaction) | • Product Manager • CS Operations |
By following this 30-day sprint, you move from abstract strategy to real-world data in just four weeks. You avoid “analysis paralysis” and gain the ability to iterate based on what your customers actually say, not what you think they will say.
If you want to see what a 30-day “Minimum Viable Agent” pilot looks like for your policy, claims, or renewal journeys, book a demo with Kommunicate.
But once the bot is live, how do you prove its value to the board?
How Should Leaders Measure ROI?
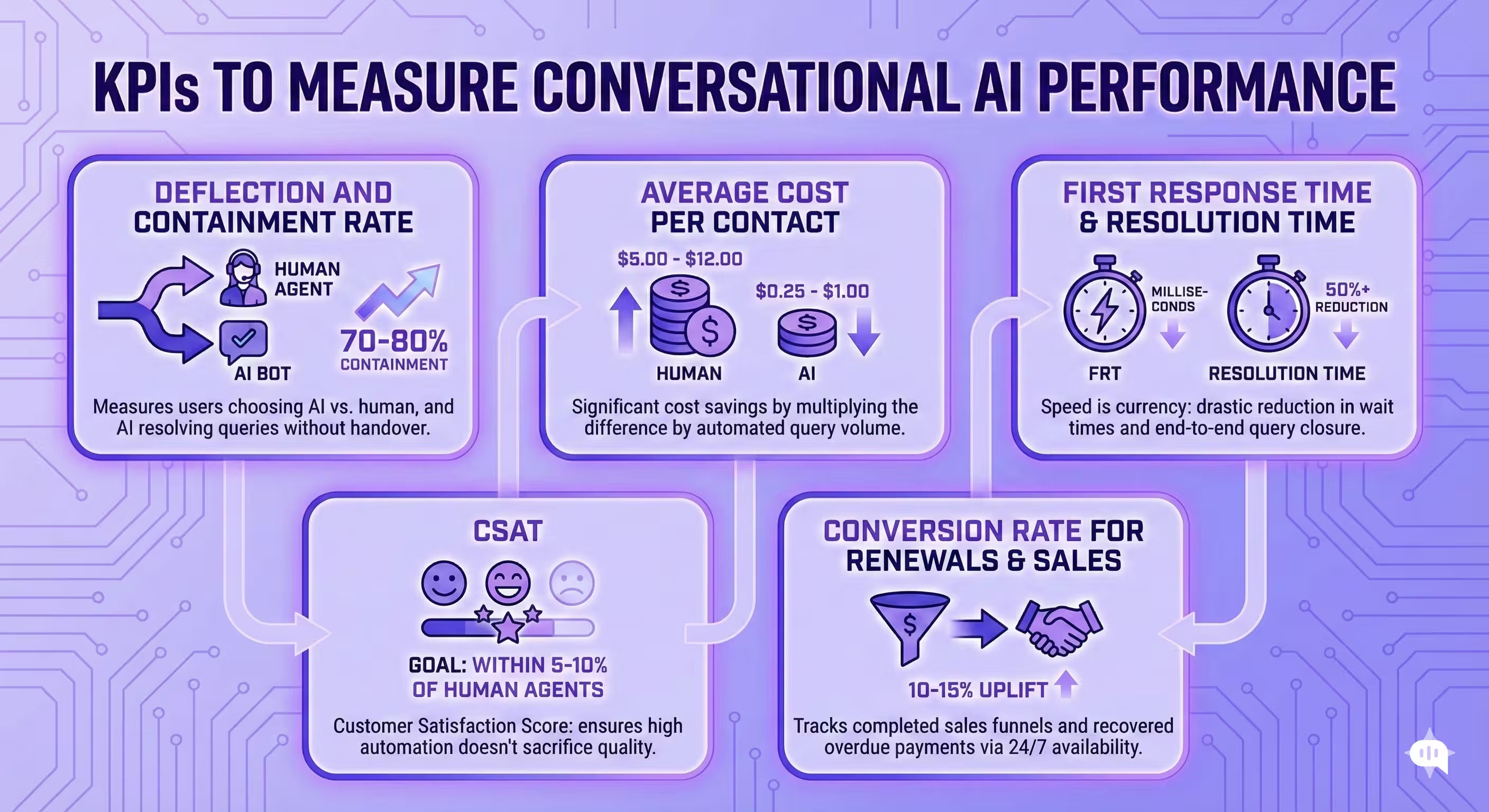
In the past, the only metric that mattered for automation was “call reduction.” Today, that is too narrow. A successful AI agent drives efficiency, sure—but it also drives revenue and retention.
To get a true picture of your ROI, you need to track these five headline KPIs.
1. Deflection & Containment Rate
This is your efficiency baseline.
- Deflection measures how many users chose the chat channel instead of calling.
- Containment measures how many of those chat conversations were fully resolved by the AI without human intervention.
- Benchmarking: For Tier-1 queries (FAQs, status checks, basic policy updates), mature programs aim for a steadily rising containment rate, with clear guardrails and low-risk intent coverage expanding over time. Track containment by intent category rather than as a single vanity number.
2. Average Cost Per Contact (CPC)
This is the most direct financial metric.
- The maths: Costs vary by region and channel, but the gap between assisted service and self-service is typically material. Gartner reported an average of $8.01 per contact for live channels (phone, live chat, email) versus about $0.10 for self-service (web/app) in its 2019 customer service research. Use this as a benchmark, then replace it with your internal blended cost per contact for a board-ready model.
- The ROI: Estimate savings as (assisted CPC – automated CPC) × deflected contacts. Then layer in secondary benefits: reduced handle time for escalations (because the bot pre-collects data), fewer repeat contacts, and higher retention driven by better claims transparency.
3. First Response Time (FRT) & Resolution Time
Speed is the currency of the digital economy.
- FRT: Should drop from hours (email) or minutes (phone hold) to milliseconds.
- Total Resolution Time: Track how long it takes to close a ticket from first contact to final outcome. Conversational AI can reduce resolution time by pre-collecting information, guiding customers to the right path, and reducing follow-up cycles—especially for Tier-1 intents.
4. Customer Satisfaction (CSAT)
High automation means nothing if your customers hate it.
- Track CSAT specifically for bot-handled conversations versus human-handled ones.
- The goal: Do not chase perfect CSAT at the expense of compliance. Instead, compare bot satisfaction against your baseline for the same intent category, and pair it with objective measures such as successful task completion and reduced repeat contacts.
5. Conversion Rate (For Sales/Renewals)
Don’t just measure savings; measure earnings.
- Sales: For quote-generating bots, track the % of users who complete the funnel.
- Renewals: For retention bots, track the % of overdue payments recovered via automated nudges.
- The impact: Availability and speed matter. When prospects can get answers instantly—especially outside business hours—conversion can improve because fewer leads drop off while waiting for a callback. Treat this as a measurable hypothesis and validate it in the pilot with A/B routing and funnel analytics.
Tracking the right KPIs ensures that your automation strategy is actually delivering business value, turning what was once a support cost centre into a driver of efficiency and retention.
But knowing what to measure is only half the battle. You also need a platform capable of executing this strategy without requiring a year-long IT project.
Where Does Kommunicate Fit in the Solution Stack?
Kommunicate is designed to reduce fragmentation across channels by acting as an orchestration layer between your backend systems and your customers—so conversations can stay consistent as customers move between web, WhatsApp, and other touchpoints.
For carriers specifically looking to deploy conversational AI in insurance, Kommunicate offers a unique blend of agility and control:
- Zero-Code Workflow Automation: You don’t need a team of engineers to build a sophisticated FNOL or quote flow. Kommunicate’s visual bot builder (Kompose) allows your product and support teams to design, test, and launch complex journeys in that 30-day pilot target.
- Deep Integration Capabilities: As we discussed, the “engine” matters. Kommunicate comes with pre-built integrations for major CRMs (Salesforce, HubSpot, Zendesk) and robust Webhook support to connect with legacy Policy Admin Systems. This means your bot can actually fetch real-time premium data and process renewals, rather than just giving generic answers.
- Omnichannel Support: Whether your policyholder prefers WhatsApp, web chat, in-app chat, or email, Kommunicate can unify interactions into a single view for agents and supervisors, helping preserve context across touchpoints.
- Generative AI With Guardrails: Kommunicate can leverage generative AI to keep conversations natural while applying controls such as approved knowledge sources, refusal rules, and escalation thresholds—so outputs remain aligned with your governance model.
- Seamless Human Handoff: Recognizing that insurance queries can be high-stakes, Kommunicate’s “Bot-to-Human” handover is best-in-class. If a user signals distress or a complex claim scenario, the system instantly routes the chat to a live agent, complete with the full conversation history and intent tags.
With Kommunicate, you get the best of both worlds: the efficiency of an AI workforce and the safety net of human oversight, all within a platform designed to scale as your needs grow.
However, even the best tools cannot fix a flawed strategy. As you prepare to launch, be wary of the common pitfalls that have derailed similar projects.
What Are the Common Failure Modes to Avoid?
Technology is rarely the reason an AI project fails; usually, it is the execution strategy. We have seen dozens of carriers struggle because they treated conversational AI as a one-time IT project rather than an evolving product.
Here are the seven most common traps to avoid:
- Starting with “The Everything Bot”: Trying to launch with 50+ intents on Day 1 is a recipe for disaster. Start with the top 5 high-volume queries and master them first.
- Letting the Bot “Guess” on Regulated Topics: Failing to implement strict refusal layers for advice-based questions (e.g., “Is this investment safe?”) can lead to compliance nightmares.
- No Integration Plan: Launching a bot that isn’t connected to your backend means it can’t do anything. If a user asks for a policy copy and the bot says, “Please call support,” you have failed.
- Poor Escalation Design: There is nothing worse than a bot that loops endlessly when it doesn’t understand. You must have a clear “escape hatch” that routes frustrated users to a human immediately.
- Ignoring the “Tone of Voice”: An insurance bot dealing with a car crash needs to sound empathetic, not cheerful. A mismatch in tone during sensitive moments destroys trust.
- The “Set and Forget” Mentality: AI agents degrade without care. If you don’t have a product owner reviewing chat logs and “retraining” the bot weekly, its accuracy will plummet.
- Burying the Bot: Placing the chat widget only on the “Contact Us” page instead of high-intent pages (like Claims or Renewals) ensures low adoption and wasted effort.
Successful automation is not a destination; it is a cycle of launching, listening, and refining.
Conclusion
The insurance industry is at a pivot point. The old model of fragmented, 9-to-5 support is no longer compatible with a customer base that lives in an on-demand, 24/7 world.
Your customers don’t want “digital transformation” in the abstract. They want to know that if they have an accident at midnight, or a question about their renewal on a Sunday, they can get an answer immediately—without navigating a phone tree.
Conversational AI offers the only scalable way to bridge this gap. By building a unified conversation layer, automating high-impact journeys, and ensuring strict governance, you can lower your cost-to-serve while actually increasing customer satisfaction.
Conversational AI is mature enough to automate meaningful parts of the insurance lifecycle—if it is designed with integrations and compliance controls from day one. If you want to validate this in your environment, book a demo with Kommunicate.
Frequently Asked Questions
Conversational AI in insurance refers to AI-powered systems that handle customer and agent interactions in natural language. These systems automate tasks such as claims intake, policy queries, renewals, fraud screening, and quote generation, either through text or voice channels, across the full policy lifecycle.
Conversational AI transforms FNOL from a phone-based, agent-dependent process into a guided, 24/7 digital workflow. The AI collects claim details, accepts photo and document uploads, assigns a claim reference number, routes the claim to the right adjuster, and provides real-time status updates.
A chatbot follows pre-written scripts and breaks when customers deviate from expected phrasing. Conversational AI uses NLP to understand intent regardless of how it is expressed, maintains context across a multi-turn conversation, connects to live backend systems, and takes action — processing requests, not just responding to them.
Enterprise insurance deployments should verify SOC 2 Type II certification, HIPAA compliance (for health insurance), GDPR data handling (for EU operations), ISO 27001 information security certification, and PCI DSS compliance if payment data flows through the conversation. Beyond certifications, the platform should support data masking, configurable data residency, and a whitelist-based knowledge architecture.
A Minimum Viable Agent targeting five high-volume intents can be live in 30 days using a phased sprint approach. Full-deployment programmes covering claims, renewals, onboarding, and underwriting assistance typically run 90–180 days depending on integration complexity and the number of policy systems involved.
Industry benchmarks suggest 30–50% reduction in routine support volume (Rasa), 80% reduction in initial claims processing time (ResearchGate, 2024), and significant cost savings given the $8.01 average cost per live-agent contact (Gartner). Revenue impact through improved renewal conversion and lead qualification is harder to benchmark generically but consistently cited as material by insurers with mature deployments.

Devashish Mamgain is the CEO & Co-Founder of Kommunicate, with 15+ years of experience in building exceptional AI and chat-based products. He believes the future is human and bot working together and complementing each other.