Updated on May 4, 2026
Estimated reading time: 19 minutes
TL;DR:
Most patient engagement software is built for digital natives and accidentally excludes the patients who need it most. Older adults represent a fast-growing share of healthcare consumers, yet they face barriers that prevent them from using the very tools designed to support their care.
This article breaks down where the design failures happen, what older patients actually need from a healthcare communication system, seven actionable design principles to close the gap, and a shareable 10-point senior accessibility audit your team can use today.
Margaret is 74. She has Type 2 diabetes, mild arthritis, and three separate providers. Last week, her oncologist uploaded an abnormal scan result to the patient portal. The system sent an automated push notification at 11:47 PM.
The notification linked to a login page that required a password reset. The reset email went to an address her daughter had set up two years ago and no longer monitored. The test result sat unread for five days.
The technology worked exactly as designed. That’s the problem.
This article follows our piece on how slow response times damage patient engagement, which showed that 62% of patients say long hold times actively discourage them from choosing a provider, and that patients with a bad communication experience are four times more likely to switch. Speed matters.
But a system that responds in milliseconds to a patient who cannot navigate the interface, cannot read the font, and cannot interpret the result is not solving the patient engagement problem.
Older patients (loosely defined here as adults aged 65 and over, though barriers begin accumulating as early as 50) represent the fastest-growing segment of healthcare consumers in the United States. They carry the highest burden of chronic disease and the most frequent need for consistent healthcare communication. They are also the group most consistently excluded by the digital systems built to serve them.
In this article, we’re talking about the invisible needs of seniors like Margaret. We’re going to cover:
- The scale of the problem: who are we designing for?
- Where do current systems fail older patients?
- What do older patients need from a healthcare communication system?
- 7 design principles for accessible patient engagement software
- The AI chatbot question: Is it helpful or harmful for older patients?
- The 10-point senior accessibility audit
- The equity argument: why this is not a niche problem
- Conclusion
The scale of the problem: who are we designing for?
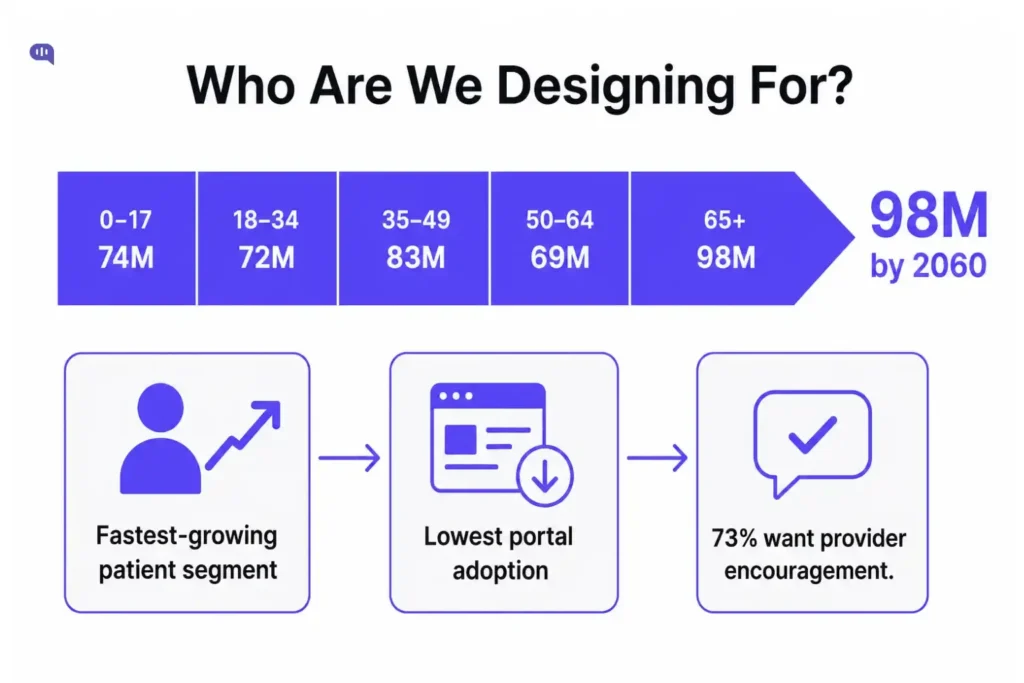
The U.S. adult population aged 65 and older was 46.2 million in 2014 and is projected to reach 98 million by 2060. The systems built for patient engagement will be the primary interface for that population within a decade.
Portal adoption has risen sharply across the general population.
A 2023 study found that the percentage of patients accessing a portal increased from 31% in 2014 to 68% in 2022 (including a 46% jump between 2020 and 2022 alone), driven partly by the pandemic and partly by federal information-blocking provisions that gave patients the right to immediate access to their health data.
Patients with cancer use portals at a higher rate than the general patient population: 45.5% compared with 38% of all patients, according to Health Information National Trends Survey data from 2019 to 2020. The portal has become a load-bearing infrastructure for healthcare delivery.
And yet older adults are systematically left out of that growth.
Portal registration and engagement drops significantly with age:
- Adults aged 70–74 and 75–79 are significantly less likely than 65–69-year-olds to be registered on patient portals
- Even among those who are registered, older adults are far less likely to have sent messages, viewed lab results, or ordered prescription refills
Among patients with cancer, portal access disparities follow the same fault lines as broader digital health inequities. Patients with persistently lower engagement rates include:
- Older patients
- Rural residents
- Non-English speakers
- Uninsured individuals
- Non-white patients
What makes this data particularly striking is that the demand is there. When older adults are asked what would most increase their portal use:
- 73% cite provider encouragement
- 69% cite guided clarification of the benefits
- 69% say they want active support during enrollment
The demand is there; it just needs design, infrastructure, and institutional follow-through.
How do portal disparities compound in cancer patients?
We looked at the BMJ Oncology state-of-the-art review (Suresh et al., 2025) to show where portal use among patients with cancer breaks down across demographic lines.
| Patient Characteristic | Direction of Effect on Portal Use |
|---|---|
| Older age | Lower likelihood of portal registration and use |
| Rural residence | Lower likelihood of portal registration and use |
| Limited broadband access | Lower likelihood of portal registration and use |
| Limited English proficiency | Lower likelihood of portal registration and use |
| Non-white race/ethnicity | Lower likelihood of portal registration and use |
| Male sex | Lower likelihood of portal registration and use |
| Uninsured status | Lower likelihood of portal registration and use |
| Unmarried status | Lower likelihood of portal registration and use |
| Severe or complex disease | Higher likelihood of portal use in inpatient settings |
| Higher portal utilization | Better concordance with care plan and stronger medical decision-making confidence |
The last two rows are important. Patients who manage to overcome the access barriers and use the portal consistently report better healthcare experiences:
- More agreement with care plans
- Stronger confidence in medical decisions
- Increased survival during chemotherapy.
Inaccessibility is not merely a UX problem. It has downstream clinical consequences. So, let’s try to understand where the infrastructure fails.
Where do current systems fail older patients?
The gap between older patients and their portal is not a gap in willingness. It is a gap in design. And it is wider than most healthcare organizations realize.
Healthcare websites had an average of:
- 6.1 keyboard accessibility violations per page
- 21.5 inaccessible form and input elements per page
- 17.2 inaccessible images per page
- 69.1 unique violations of WCAG minimum color contrast requirements
This directly prevents older patients from reading test results, medication instructions, or emergency contact information. These are not edge-case issues. They are the baseline.
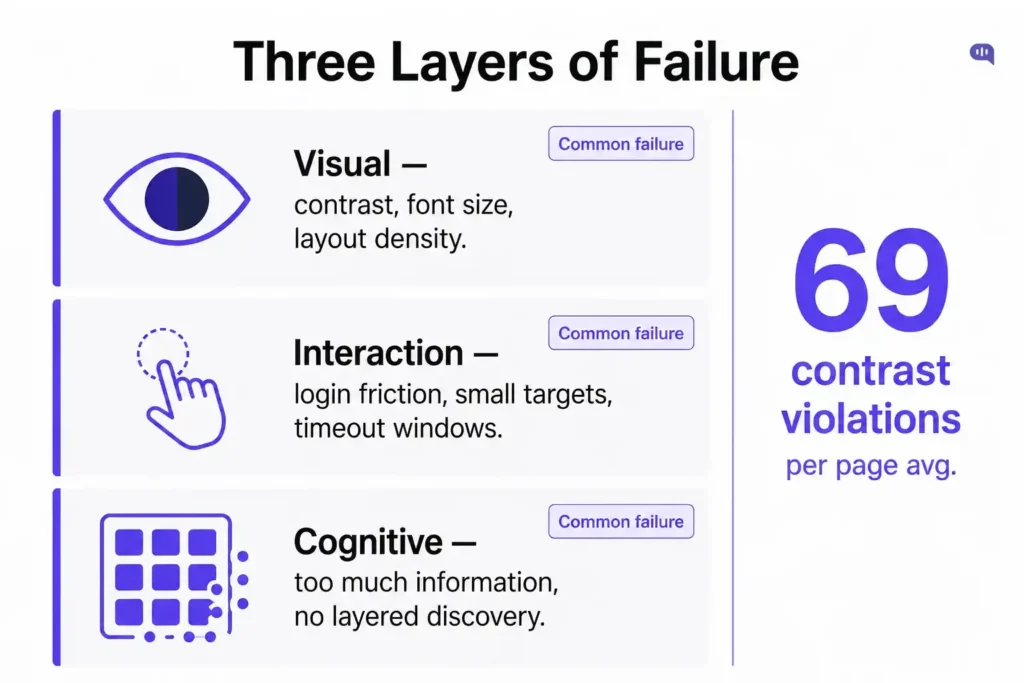
The failures cluster into three distinct layers.
Visual design failures
Color contrast is the most cited and most frequently violated accessibility requirement. WCAG 2.2 requires a minimum contrast ratio of 4.5:1 for normal text and 3:1 for large text (requirements that, according to a 2024 WebAIM analysis, are violated on 83.6% of websites). For patients experiencing age-related vision changes, which begin affecting most adults in their 50s, insufficient contrast can make test results, medication dosing, and appointment details effectively unreadable.
Font size is a companion issue. WCAG 2.2 requires that text be scalable up to 200% without loss of content or functionality. Most healthcare portals either use fixed font sizes or break their layout at scale. Text spacing requirements are routinely ignored.
These are not aesthetic preferences. They are functional barriers.
Interaction and navigation failures
WCAG 2.2 introduced enhanced focus indicator requirements specifically because many people cannot see small changes in visual appearance. Focus indicators must now meet a minimum size threshold and a 3:1 contrast ratio against their background. This matters enormously for patients with reduced fine motor control or early cognitive decline who rely on keyboard navigation.
Login flows are a particularly acute failure point.
Among older adults surveyed, initial portal setup was cited by
- 36% as a primary barrier
- Sign-on difficulties by 32%
- Information sharing by 35%
Two-factor authentication, mandatory password complexity, and session timeout windows that are too short all create dropout points before a patient ever sees their health information. The survey also identified typing difficulties, small icon sizes, and difficulty safely sharing portal access with caregivers as compounding friction.
Cognitive overload
One of the greatest enemies of patient engagement is cognitive overload. Presenting a patient with a dense dashboard full of test results, pending tasks, care plan items, and billing notifications all at once leads to what researchers have described as “disengagement by data.”
For older adults managing multiple chronic conditions, an overwhelming interface is often the last interface they try.
The result of these three failure layers is a kind of invisible exclusion. No single barrier is insurmountable in isolation. But stacked together, they produce a patient who gives up. Not because they didn’t try, but because the system never made it easy enough to keep trying.
Which is why it’s necessary to look at healthcare communication systems and see if it matches the needs of the most vulnerable.
What do older patients need from a healthcare communication system?
Understanding the barriers is necessary. Understanding what older patients are actually asking for is where design starts.
1. Time and space to think
Traditional virtual engagement forces patients into high-pressure, time-bound interactions. Asynchronous engagement does the opposite. By giving patients a window to engage with information at their own pace, healthcare organizations support the slower, more deliberate thinking that produces better health decisions and more accurate responses.
This is not a concession to cognitive decline. It is a good communication design for anyone dealing with complex, emotionally charged medical information.
2. A human always within reach
Patients often feel more confident knowing they can reach a real person when something goes wrong. Live chat with medical coordinators, clear help sections with troubleshooting guides, and phone numbers visible on every screen are foundational trust signals for older patients.
Leaving a patient in a dead-end error message, or forcing them to leave the platform entirely to find support, is a clinical risk dressed up as a UX problem.
3. Caregiver and family access
Secure messaging with clinical teams has emerged as a key function of portal use among patients with cancer. Care partners also use secure messaging, though often without properly setting up proxy accounts because the proxy process is not well communicated or easy to complete.
Proxy account use among older patients remains very low, suggesting limited awareness of this functionality.
Care partners who use the portal to manage their own health are more likely to use it effectively to manage care for someone else. That knowledge transfer starts with an onboarding process that treats caregiver enrollment as a default, not an afterthought.
4. Provider encouragement as a catalyst
73% of older adults said provider encouragement would most effectively increase their portal use. Not a better app. Not a simpler login. A clinician telling them it was worth their time.
Health technology navigators working with older and linguistically diverse patients in a Los Angeles safety-net system described their most effective moments not as technical troubleshooting but as relationship-building.
The lesson for healthcare organizations is that digital engagement for older patients cannot be purely self-service. It requires a human touchpoint who actively bridges the gap.
These needs can be mapped onto specific design principles that patient engagement software uses at scale.
7 design principles for accessible patient engagement software
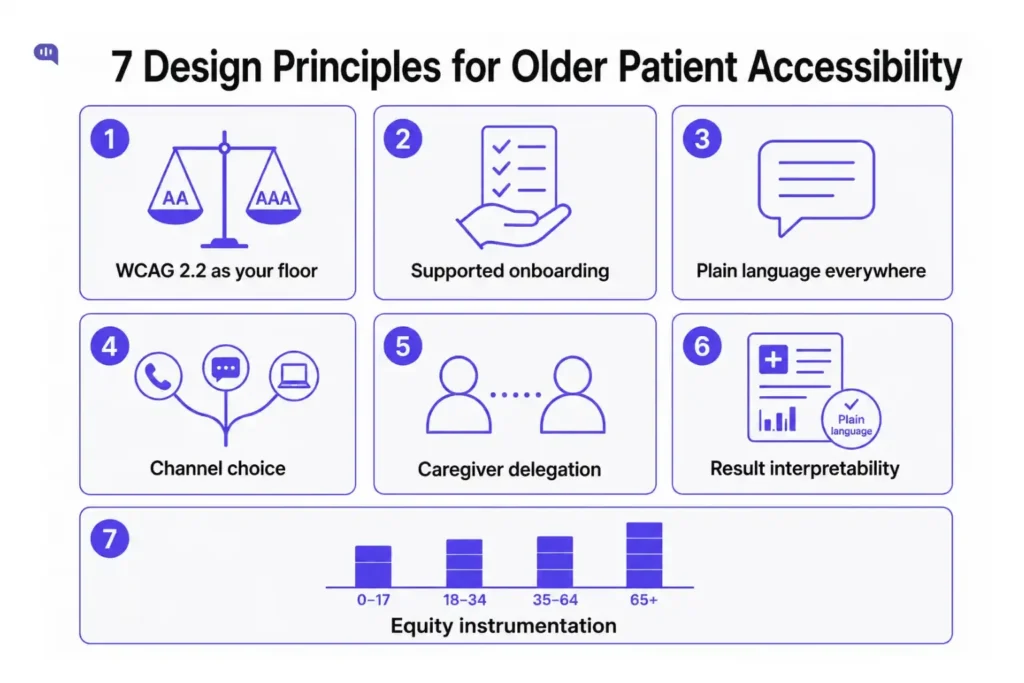
These principles are ordered by impact, not complexity. Some require developer time. Others require only a willingness to look at the interface through a different patient’s eyes.
1. Meet WCAG 2.2
WCAG 2.2 is the legal and ethical floor, not the design target. For a healthcare interface used by older adults, the minimum contrast ratio of 4.5:1 for normal text is a starting point. Font sizes should be set with relative units, so they scale with user preferences. Text spacing should meet or exceed the recommended thresholds. Interactive elements should have touch targets large enough for users with reduced dexterity.
The practical implication: run your portal against a WCAG 2.2 automated checker before each release. Then have an actual older adult try to complete a core task without assistance. The automated checker will catch the measurable violations. The human session will catch everything else.
2. Redesign onboarding as a supported journey
Account creation should be fast, intuitive, and free of medical jargon. Instructions should be written at or below an eighth-grade reading level. A short welcome video that introduces the three most important portal tasks reduces abandonment and reinforces credibility.
The navigator research takes this further. The most effective onboarding for older patients in safety-net settings was not technology-led. It was human-led, with a trained community health worker walking alongside the patient through initial registration and first use. For healthcare organizations that cannot staff navigators at scale, a structured video call or phone walkthrough at the point of enrollment comes closest to replicating that effect.
3. Write in plain language throughout
Medical jargon is a documented barrier for older patients, particularly those managing multiple chronic conditions where the volume of clinical language is high. The CDC’s plain language guidelines offer a practical framework: use active voice, short sentences, common words, and concrete examples.
The test result context is where this matters most acutely. Among patients with cancer, 98% wanted access to their oncology notes.
The research-supported resolution is not to gate the information, but to add interpretive layers: a plain-language summary at the top of every result, a tooltip that explains what the value means, and a one-tap pathway to ask a question. Immediate access without an accessible explanation produces anxiety. Immediate access with layered interpretation produces engagement.
4. Offer channel choice
Not every older patient will use a portal. Some will never feel comfortable with an app. And that is a legitimate preference, not a failure to be corrected.
Voice AI technologies are being adopted rapidly by U.S. healthcare organizations, with 63% already piloting or using them to improve patient engagement and reduce costs, according to a 2025 Deloitte report.
Medication adherence tools with voice-enabled interfaces improved adherence by 22% in elderly patients in one documented deployment. For appointment reminders, medication check-ins, and post-visit follow-ups, AI voice channels often outperform portal messaging for older adults.
The design implication is not to choose between portal and phone. It is to build both, integrate them into a single patient record, and let the patient choose their preferred channel at enrollment rather than at the point of need.
5. Build caregiver delegation into the default enrollment flow
Proxy access should be offered at the point of first enrollment. The enrollment process should ask: “Is there a family member or caregiver who helps you manage your health? Would you like to give them access to your portal?”
Care partners benefit substantially from portal access. Those who use the portal to manage their own health are more likely to use it effectively to manage care for someone else.
6. Solve for result interpretability
The 21st Century Cures Act gave patients the right to immediate access to their health information. That was a meaningful policy change. But it created an unintended consequence: patients now regularly view test results before their clinician has had a chance to review or contextualize them.
The majority of patients prefer this immediate access, and most clinicians and patients agree that routine results should continue to be released through the portal immediately. But some patients find radiology reports confusing, and care partners of patients with cancer said results were easy to misinterpret without guidance.
7. Instrument for equity
Most patient engagement platforms track overall engagement metrics. Few track those metrics disaggregated by age, language, and geography. The result is that equity gaps are invisible until they surface in outcomes data.
Building age and language filters into standard engagement dashboards allows healthcare organizations to see the gap in real time and intervene before it compounds.
Portal use was associated in research with patients with cancer feeling more in agreement with their care plans, having better access to high-quality health information, and improved confidence in medical decision-making, but those benefits only reach patients who can use the portal in the first place.
These design principles offer a way forward in terms of accessibility for older patients. But, for healthcare executives, there is another larger question. That is around AI and what it means for equity in patient engagement.
The AI chatbot question: Is it helpful or harmful for older patients?

Patient engagement platforms are increasingly built around AI-powered chatbots as the first layer of interaction. For older patients, this introduces a specific set of design considerations.
61% of patients still struggle with chatbots
In a survey of 617 patient chatbot users, 35% felt they could not fully understand the chatbot, and 61% felt the chatbot did not completely understand them.
Those comprehension gaps are steeper for older adults, for whom ambiguous phrasing, unexpected error messages, or long response delays trigger disengagement or confusion.
A chatbot that does not understand a patient’s question is worse than no chatbot at all for this population.
What works: Adaptive chatbots
The most effective AI interfaces for older patients share three characteristics:
- Shorter, plainer sentences — Medical jargon is replaced with common-language alternatives, and responses are broken into digestible steps rather than blocks of text
- Proactive escalation — When a conversation pattern suggests confusion (repeated questions, non-sequitur responses, long pauses), the system initiates a human handoff rather than waiting for the patient to ask
- Voice as a primary channel — AI voice interfaces bypass the entire text-interface problem for patients who find typing, reading, or navigating on a screen difficult
The non-negotiable: always a path to a human
No AI-first engagement system for healthcare should leave an older patient in a conversational dead end. A live human should be reachable in one step from any point in the conversation immediately and visibly.
For older patients, this is not a UX nicety. It is a clinical safety consideration. A confused patient who cannot reach a human through the portal will call the practice, clog the phone line, or simply disengage. Each of those outcomes is worse than the alternative.
Now that we understand the landscape and have a plan to build a more accessible UX for older patients, let us give you a simple playbook that you can use to run an audit.
The 10-point senior accessibility audit
Use this checklist to evaluate your current patient engagement software against the most common barriers facing older patients. It is designed to be completed in a half-day audit session with one product team member and one or two older adult users who have not previously used your platform.
Try the 10-point Senior Accessibility Audit below to evaluate whether your patient engagement software is usable for older patients.
10-Point Senior Accessibility Audit — Kommunicate
The Senior Accessibility
Audit for Patient Engagement Software
A 10-point checklist to evaluate how well your patient communication platform serves older adults. Complete each item and get an instant score with priority actions.
Full breakdown
This will give you an action plan to build a truly accessible patient engagement system in your business. Finally, to help you present the accessibility project to your board, we’ve put together a small argument that has worked for our healthcare clients like Amgen and Amref.
The equity argument: why this is not a niche problem
It is tempting to frame older patient accessibility as a segment-specific challenge.
However, low-income, rural, and geriatric patients are the groups most affected by the digital divide in healthcare. They are simultaneously the groups with the highest chronic disease burden, the most frequent need for ongoing provider communication, and the least access to the support infrastructure that helps higher-resourced patients navigate digital systems.
A significant portion of the U.S. population does not live within catchment distance of a comprehensive cancer center. For those patients, telehealth and digital engagement tools are not a convenience. They are the primary access pathway to specialist care.
Telehealth during the COVID-19 pandemic was accepted by patients with cancer as a substitute for many in-person visits that did not require a physical examination. But telehealth continued to exacerbate disparities. The technology expanded access for the patients who were already well-served and widened the gap for those who were not.
That pattern is predictable when accessibility is treated as a feature rather than a foundation. And it is reversible when accessibility is designed in from the beginning.
There is also a straightforward commercial argument that is often underemphasized: older patients have:
- The highest healthcare utilization rates
- The longest chronic care relationships
- The greatest need for consistent communication across multiple providers and care episodes.
Retaining an older patient through an accessible engagement experience is not a charitable act. It is one of the highest-return investments a healthcare organization can make.
Conclusion
Most patient engagement software is not inaccessible because its designers set out to exclude older patients. It is inaccessible because those designers never meaningfully included them.
The problems described in this article are not exotic or expensive to solve. They are documented, well-understood, and fixable with existing tools and standards. WCAG 2.2 provides the technical specification. Plain language guidelines provide the content framework. Navigator research provides the implementation model. The audit checklist above provides the evaluation mechanism.
What is required is the organizational decision to treat older patient accessibility not as a compliance checkbox or a future roadmap item, but as a current design constraint.
A system that is fast but inaccessible has not solved the patient engagement problem. It has just surfaced it more efficiently. The goal is a healthcare communication system that meets every patient exactly where they are.
Want to see how Kommunicate’s patient engagement platform approaches accessibility and multichannel communication for older patients? Book a demo

Devashish Mamgain is the CEO & Co-Founder of Kommunicate, with 15+ years of experience in building exceptional AI and chat-based products. He believes the future is human and bot working together and complementing each other.